Hello hello!
My last 5 weeks of second year have been filled with Alternative Practice Placement programme. This program comprised of lots of opportunity to do self learning and some group work both online and on campus so it had a blended learning approach.
Week 1 involved completing the practice supervisory NES units via Turas in preparation for our days as Practice supervisors and Practice Assessors once we qualify. There were times when working through this I wondered if it was too soon to be learning this but I guess our time to be PS/PS is not that far around the corner and it will be of great benefit come that time. After all sharing skills, knowledge and experience and learning to students and colleagues is the responsibility of all nurses as per 9.4 of the NMC code. The modules covered the following: the NMC (2018a) standards for student supervision and assessment, how the roles of PS, PA and academic assessor (AA) work together to supervise and assess students and the responsibilities of the PS and PA and what this means for our practice. It looked at learning theories, learning styles and preferences and ways in which to empower the student nurse to be an independent learner. The modules also covered the quality standards for practice learning and emphasis the importance of a conducive learnign environment for student nurses to learn efficiently to support their development of safe and effective person centered care. “The NMC (2018b) expects that PLE’s are safe and effective and provides guidance for approved higher education institutes (HEIs) and their practice partners to adhere to within the standards. They also provide supporting information to support organisations when developing and maintaining PLE’s”. Educational Audits are a tripartite process, normally undertaken by the following representatives: practice area usually the Senior Charge Nurse (SCN), Team Leader (TL), or manager for the area or their deputy, health board practice education team, e.g. PEF/CHE and higher education institutes. Audits are undertaken via the QMPLE data base which was designed by NHS education for Scotland (NES). This was a really interesting part of the training to learn about. It covered the role of the PS/PA and their differences. It covered the participation in care framework which is a visual representation of student development as they progress in practice learning from dependant to developing independence to independent. It covered models of coaching and a small section on supporting equality and diversity and reasonable adjustments. I feel that there needs to be more input and innovation into this section for PS/PA’s to support student nurses who do have alternative learning requirements. The modules provide support on how to assess student nurses as a PS/PA and addressed the roles, responsibility and accountability as a PS/PA in terms of assessment. The last section looked at supporting learners and how best to respond to student conduct and proficiency. This is definitely a resource that I will refer back to and refresh after I register.

Week one also involved completing the annual RGU Student led Learning disability conference material and attended the live Q and A event.

This years conference aimed to follow on from last year’s conference called “Out of the Shadows” which I had the honour to be apart of. Last years conference focussed on the post-pandemic recovery and experiences of individuals with a learning disability and their families. This year’s conference looked at how healthcare professionals can be the ‘light’ for families and service users, instil family centred care and continue to advocate for promoting health care access and services that can bring about positive lasting changes. The speakers included Dr Heather Bain with the introductory speech, Isla Mcglade with the keynote speech, Billy Ridler with a paramedic perspective, Jamie McCallum (father to Rosie and founder of Wouldn’t change a thing charity), and Elaine Scougal mum to Ollie and Cam. Both are both amazing parents who feature in the conference every year, and are fantastic. 🙂 Liam Waldron (lecturer at RGU who brought a spiritual care perspective to this conference. Jackie Stewart Registered Learning Disability Nurse. Kerry Anderson Registered Learning Disability Nurse. Lucienne Cooper and Claire Hodge founder of positive about down syndrome charity, and it ended with a closing speech from professor Susan Dawkes the head of the school of nursing midwifery and paramedic practice at RGU. It was a very insightful conference packed full of learning. My favourite presentations where Jamies, Elaine Ollie and cams and Liam’s one! 🙂 Learning disability’s is an area that I am particularly passionate about so it was really great to complete the material and learn from the guest speakers this year. I am looking forward to next years one already!
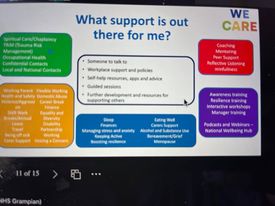
Week 2 started with a session delivered by the NHS Grampian We Care Team/ We Care Kindness Project which focussed on resilience and wellbeing as professionals. We Care is a hub where you can access information, help and advice related to you and your teams physical and mental wellbeing You can follow them here https://www.twitter.com/GrampianWeCare

The session looked at what mental health and wellbeing meant to us, and gave us a chance to think about how we could recognises if we were stressed and/or if our colleagues were stressed. It gave as an opportunity to reflect on our own stress levels using the stress level bucket and how we could use that in the work place. It highlighted the impact of stress within the health care work setting and highlighted the 5 ways to wellbeing. It was a nice little session. Prior to the session we had the opportunity to answer questions about resilience to get us into the frame of mind for the session in the afternoon. I really liked this little session it has prepared us for life as a registrant!
We had a session with Lead Chaplin and head of spiritual care Gillian Douglas. Gillian covered the who, what and why of spiritual care, bereavement and loss and the grieving process and chaplaincy in the NHS. We explored how spiritual pain care be identified through behaviours and questions such as anger directed at god or other people, bitterness- what have I done to deserve this? Regret- I should have been a better person. Guilt and punishment- have done something wrong?. We looked at what we can do to help; some individuals may want to talk others may not. Key questions to ask might be : what things are are most important to you?, what helps? What makes it worse? Would you like someone to talk to? We learnt that spiritual care is not just delivered by chaplains but nurses too. We explored some models of grief and how we can support people during these times. Following on from this session we undertook some death and bereavement educational resources on TURAS.
We had a session with Rachel Holland practice educator NHS Grampian. This session involved looking at CYP assessment using ABCDE, family centered care and safe guarding and GIRFEC. This was a well rounded session about CYP. Following this session we worked on Child protection modules on TURAS, we utilised the spotting the sick child resource which has lots of great little quick videos about assessing children and different conditions seen with CYP’s. I say they were quick videos but the website was being used by my whole cohort and the rest of the world making the site a bit on the slow side lol. This is a resource I will definitely utilise in my CYP year!

We had a session about adrenal insufficiency steroid education. This was an interesting session. We spoke about steroid reliant conditions and the importance of steroids for these individuals survival.
During our independent study days we created case studies. Over the 2 weeks we had independent study I created one that combined two conditions. It was based on a fictional patient who had type 2 diabetes and sepsis.
Name – John Jargon
Age- 82
History- John Jargon is an 82-year-old man who lives on his own. He has a history of poor healing of wounds and is overweight.
Symptoms- John presented to ED with a rapid pulse and breathing, and downiness and a sweet-smelling odour on his breath. Once stabilising John, he said to have frequent urination, increased thirst and hunger and was feeling extremely lethargic and complained of blurry vision on and off for a few weeks. He was diagnosed with Type 2 diabetes. He has suspected sepsis (site of infection is the poor healing wound).The wound is showing signs of swelling, redness, pain and producing exudate..
In my case study I included some facts and figures about both conditions, investigations to be carried out, aetiology, signs and symptoms, pathophysiology and pharmacology for both conditions and filed in a NEWS observations chart with hypothetical/probable readings. I included some management strategies and a suggestions for discharge. This was a great opportunity to revise some science as well as nursing care.

Week two ended on some virtual group work and peer to peer teaching on Fluid balance charts. We came to the conclusion as a group that there are so many different ones! But we knew Input and output should balance the same somewhat.

Week 3 started off with a session on campus in the skills lab. This involved working in little groups to do medication management, assessing care, planning care, implementing care and evaluating the care of a fictional patient. We also practiced manual pulse. This session was a helpful refresher, it would have been good to have some other skills in this session too in preparation for year three.
We had a session on Infant feeding which was really interesting. I was astonished by the impact of breast feeding which could can see on the slides below. Following this session we completed Unicef turas module and the maternity standard turas modules. We also had a session with the unity specialist midwives from Megan Blande about supporting vulnerable families in childbirth.
We had a session with ARCHIE bereavement network who spoke about the work they do and the impact covid has had to children who faced bereavement. Following on from this session we worked through palliative care resources and carried out research surrounding this area.

We had a session from the bowel and bladder specialist service which was excellent. I found this really interesting. They covered incontinence, causes of incontinence, they covered the physiology of the male and female urinary tract, types of incontinence, how the bowel and constipation can lead to incontinence, how to promote bowel health and ways to supporting people.
We had a session with Katie baxter about contextualising the future nurse roles and responsibilities which followed on from some of the work we did in week one surronnded the role of PS/PA as a registrant.

Week 3 finished with another clinical skills session on campus. This was my favourite in person session of the whole 5 weeks. We were asked to teach our peers about peak flow. I worked along side a great group of people this day and we produced a really great exhibition about peak flow to our peers and we received some great feedback from the facilitator. I was pleased to have carried out research in the morning prior to the session about peak flow and brought it with me which helped me and my group plan our teaching session for our peers.

Week 4 started by completing some trauma informed care resources through NES E-learning. Trauma informed practice is vital knowledge for all fields of nursing. The 5 principles of Truama informed care can be seen below.
- Safety.
- Trustworthiness.
- Choice.
- Collaboration.
- Empowerment

We carried out some Turas learning about the aseptic technique, wound care management and prevention of pressure ulcers and following this we had a session with the tissue viability nurses which was great. It was a very interactive session which made it really interesting and consolidate learning. This also covered more learning on the SSKIN bundles and recognising grading of pressure ulcers.
SKIN
SURFACE
KEEP MOVING
INCONTINENCE
NUTRITION & HYDRATION
A patients most vulnerable areas are:
B – Buttocks
(ischial tuberosities)
E – Elbows/Ears
S – Sacrum
(bottom)
T – Trochanters
(hips)
S – Spine/
Shoulders
H – Heels
O – Occipital Area
(back of the head)
T –toes
What we should look and feel for?
• Redness/erythema – non-blanching
when finger pressure applied
• Pain, soreness
• Warmer or cooler area over bony
prominence
• Sponginess feeling
• Hardened area
• Discolouration – dark red, purple, black
• Broken skin/ulcer
We were due to have a session about Motor Neurone disease however the session was unable to go ahead and therefore we carried out some self study about Motor Neurone disease. I found some great resources.

https://www.rcn.org.uk/clinical-topics/neuroscience-nursing/mnd-resource#limbsymptoms
https://www.mndscotland.org.uk/what-is-mnd/useful-links-and-resources#forprofessionals
Our peer to peer to peer group sessions for this week was about hand washing. We split ourselves into 2 smaller groups and each prepared a little teaching session on hand washing. We felt pretty clued up on hand washing before starting the work but unknown to us there was things about it we hadn’t thought about like there are different types of hand washing!
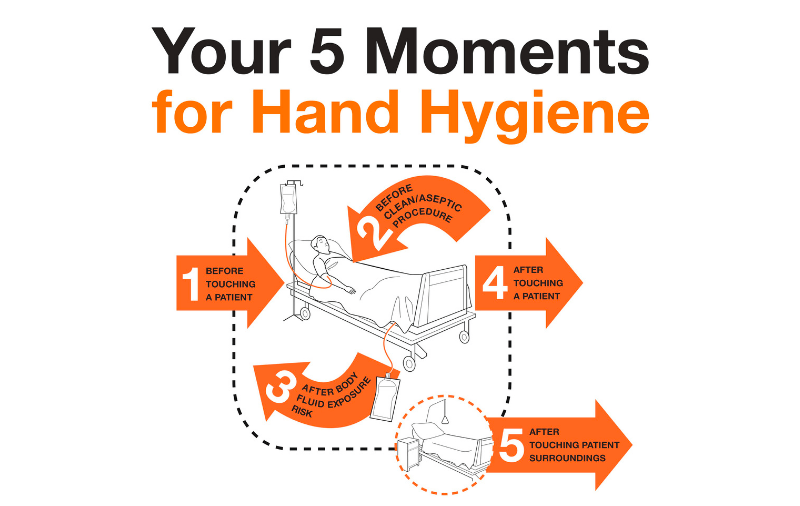
“Researchers estimate that if everyone routinely washed their hands, 1 million deaths a year could be prevented”
Week 5:
In the final week there was group project work scheduled however I was given permission to attend the RCN student committee meeting which included bundles of nursing related learning and collaboration within the team.

We had a session about care management and the work that this service offer. They covered what care management is, the purpose of the role, and what they do in the role, the skills and competency of the individual in the role, a bit about the role within the hospital and where they cover, and they provided an example of a referral. It was an interesting listen.

We had lots of suggested Turas modules to complete to make up our hours too so week 5 was an opportunity to work on some of the ones that needed finished.
To finish up the 5 weeks we had an evaluation session with the module team to sum up our experience and offer us an opportunity to feedback. This involved using the ROSE, BUD and THORN approach which I hadn’t heard of before but thought was a really good idea.

I think there was a lot of great learning offered in this learning experience. I liked the interactive sessions best as I learn by doing and visualising.
It is evident the team put oodels of effort into building this timetable and delivering the experience, so I would like to thank everyone who participated in the making of this!
This closes stage 2 to an end. Heres to year three S20 cohort! 🙂